I’VE RECENTLY BEEN SPENDING TIME ON VARIOUS FERTILITY MESSAGE BOARDS AND FORUMS, in an attempt to find out about people's most pressing concerns and questions. One topic that comes up a LOT is the IVF egg collection procedure. There seem to be three types of question:
- Questions about pain (both during and after the procedure). “Is IVF egg collection painful?” “How long did it take you to recover from egg collection?” “Is it normal to have pain after egg retrieval?” “Do most people get bloated and constipated after egg collection?” “Did you get OHSS after egg retrieval?” And so on.
- Questions about the eggs. “How many eggs is a good number?” “Can I still have success when just two eggs were collected?” “What size should my follicles be before egg retrieval?” “How do the doctors decide when my eggs are ready?” Etc.
- Questions asking for general tips and advice. “Egg collection tomorrow! Any tips/advice?” “Do I need to prepare for egg collection?”
Well… this article aims to answer them all and more! Here goes…
How will the doctors know when it’s time for my eggs to be collected?
You’re ready for IVF egg collection when your scans show that the lining of your uterus is nice and thick, and you have a decent number of follicles that are the right size. (Your eggs are microscopic in size and can’t be seen on the scan, so the size of each follicle – which encases the egg – is used as a proxy for egg size. Read this article for more about the difference between eggs and follicles.)
What size should my follicles be for IVF egg collection?
Doctors like to see follicles that are approximately 15–24mm in diameter, because these follicles will contain eggs that are deemed ready for ovulation.
Most doctors actually prefer to wait until at least a few follicles have reached at least 18mm: at 15mm, the eggs inside still might not be ready for ovulation. On the other hand, the follicles can’t be left to grow for too long: go past 24mm and there’s a risk that the eggs will be too “ripe” and therefore can’t be used.
What’s a good number of follicles?
If you have at least ten follicles that are a decent size (see above), chances are your doctor will be happy: that’s enough follicles for there to be a good chance of at least one high-quality egg inside, but not SO many that you’re at risk of severe ovarian hyperstimulation syndrome (OHSS).
Basically, you want not too many but not too few follicles, which aren’t too big or too small. “Picky” is a word that comes to mind.
I don’t have many follicles! Is egg collection doomed?
No – definitely not! You only need one fabulous egg to create one fabulous embryo, after all. Your chances of successful fertilisation might be reduced, but you’re definitely not a lost cause. (And remember: plenty of people with a large number of follicles – and therefore eggs – have ended up disappointed that not one of them fertilised successfully.)
I have a ton of follicles and I’m scared about getting OHSS!
Your doctor has a variety of methods to prevent OHSS – or at least lower the severity of the symptoms associated with it – and you can read all about them here.
Bear in mind that you might get OHSS despite all precautions, so it’s important to monitor yourself closely for symptoms. What’s more, some people get OHSS despite having close to zero risk factors. Basically, everyone needs to keep an eye out for OHSS.
I’ve been told I’ll need to take a “trigger injection” before IVF egg collection. Why? What does the trigger injection do?

Your eggs need to go through one final stage before they’re ready to be collected: they need to complete a process of maturing called “meiosis”, which in turn causes ovulation to happen.
The trigger injection kickstarts this process, and you'll need to administer it at a very specific time – usually 36 hours before your appointment for egg retrieval.
Why 36 hours? It’s because ovulation will take place approximately 36 hours after the trigger injection gets into your system (which takes a bit of time in itself). The doctors need to collect those eggs just before ovulation takes place, but just after the eggs are fully developed and ready. It’s a teeny tiny window of time, and you can’t miss it.

Questions to ask your doctor at every stage of IVF treatment: free downloadable guide
IVF isn’t just overwhelming; it can also be a mind-boggling and sometimes terrifying experience because there’s so much to learn and so many rules to follow.
Problem is, doctors are busy – and they often don’t have the time to anticipate your concerns and provide all the information you might need.
This downloadable guide contains questions that will help you understand the process better, get the answers you deserve, and feel more in control of the situation (and your rights as a patient).
Enter your email address to receive it right away.
I won't send you spam. Unsubscribe at any time.
How do the doctors determine which trigger shot I should have?
There are two main types of trigger injection:
- The hCG trigger injection, which is usually (but not always) used by people who’ve been on the long protocol. Brand names include Ovitrelle, Pregnyl and Choragon.
- The GnRH agonist injection, which is usually (but not always) used by people who’ve been on the short protocol. Brand names include Lupron and Synarel.
What happens if I forget to do the trigger shot at the right time?
Tell your doctor: they may decide to delay your retrieval by the same amount of time. Even if you’re late by ten minutes or so, tell your doctor to be on the safe side. The good news is that the teeny tiny window of time mentioned above is still a window – not a letterbox (worst analogy ever?) – so there’s room for a bit of timing leeway when it comes to the trigger and egg collection.
What happens after the trigger injection?
The countdown begins until IVF egg retrieval time! As mentioned above, you’ll have been given a specific time to arrive at the clinic/hospital, which will be a specific number of hours (usually around 36 hours) after the trigger injection.
I’ve been told to fast the night before my egg retrieval. Why?
If you’re being sedated or anaesthetised for your egg collection, you’ll be told to fast from midnight the night before – including chewing gum and sweets – and to stop drinking four hours before the procedure. Why? Because food or drink in your system can cause something called “aspiration”. I won’t explain it all here, but Google it if you want the deets.
How do they actually “collect” my eggs?
Here’s what happens:
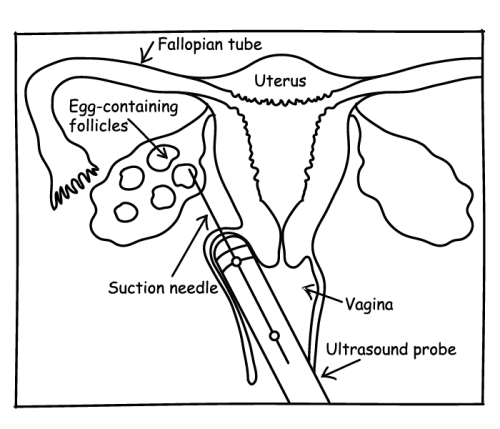
- They’ll pass a needle through the top of the vagina to get to the ovary and follicles. Ultrasound guidance helps them find the exact spot.
- Next they’ll “puncture” (my word, not theirs) the follicles so that the eggs detach from the follicle walls and can be sucked out of the ovary.
- You’ll wake up feeling a bit crampy, a bit moody, and possibly a bit hungry.
- You’ll then be told how many eggs were retrieved and how good the sperm sample looks.
- After that, it’s time to go home and REST!
Meanwhile…
I haven’t mentioned what your partner’s up to while your precious insides are being poked and prodded by a massive needle. He’s having a marvellous time: watching porn, reading fetish websites, fantasising about Scarlett Johansson and jizzing away happily in his own private wank-off room.
(That's not quite true – and many men find the sperm collection process to be quite an ordeal. If your partner is worried or has any questions, send him a link to “Sperm collection: what you need to know (an article for the men)“.)
What does IVF egg collection feel like? Is it painful?
I visited an IVF forum and asked fellow members a bunch of questions about their own egg-collection experiences. Below is what they said about the pain associated with the procedure itself, grouped according to the type of sedation/pain relief they had. You might want to be aware that NICE recommends conscious sedation for the procedure (“Women undergoing transvaginal retrieval of oocytes should be offered conscious sedation”), but very few people (in my survey, anyway) seem to have chosen or been given that option.
People who had a general anaesthetic had this to say about the procedure:
- “It felt like I just had an amazing sleep.”
- “Was asleep so can’t really comment on the procedure itself.”
Those who had heavy sedation:
- “The procedure itself wasn’t painful in the slightest. The heavy sedation pretty much felt like a general anaesthetic, and I don’t remember a thing about it.”
- “They called it sedation but I believe I was completely out both times. I found it very straightforward and not really painful.”
- “I didn’t feel a thing.”
- “I was completely out. I don’t remember much about it. I think it was fairly quick, though.”
- “I don’t remember much at all, apart from being aware I was in the room.”
- “When I was sedated I felt poking and prodding, and was a little uncomfortable.”
- “It was easier than expected. I went into hospital at 7.45am and was back home for 11am.”
- “No pain, thankfully. I was completely knocked out each time. Took about 30 minutes. The first four times [I had the procedure] I woke up in a chair in the ward – no clue how I’d moved to the chair. The fifth time, I woke up in theatre as they’d kept me in for monitoring with an irregular heartbeat.”
- “I slept through the whole thing – apart from a brief moment when I woke up to hear them say ‘There is no egg.’ This must have been one of the empty follicles, and I’d woken up at just the wrong time. When I came round afterwards, I remember saying to my hubby that it hadn’t worked – there weren’t any eggs. So when they told us they’d collected 11, I was over the moon.”
- “I don’t remember a thing.”
- “Didn’t feel a thing! Procedure was fine – only took around 15 minutes.”
- “I was completely out for the count.”
Those who had conscious sedation:
- “Egg collection wasn’t nice. I was awake the whole time. I had a drip in my arm where the pain relief was administered. I had to ask for more. I was so glad when it was all over.”
- “I was given wakened sedation, but was completely out for the whole procedure. It was absolutely fine.”
Those who had a local anaesthetic with gas and air:
- “There was an initial sting with the local anaesthetic, but after that it was fine – easier than expected. The only thing I hated was hearing them count the eggs after they came out. I was fixated on it after the disappointment of the first round, and this stressed me out more than anything else. I also wasn’t too chuffed with the doctor/nurses having a chat right in front of my stirruped legs without any dignity sheet in place!”
What happens to the eggs after they’ve been collected?
A few hours after egg retrieval (and depending on the sperm sample), they’ll be mixed with the sperm. If you’re having ICSI, a single sperm will be injected into each mature egg.
The day after the eggs and sperm have been mixed, they’ll be checked to see how many have fertilised (approximately 70% of eggs fertilise normally). At this stage they’re called embryos, and they’ll be monitored constantly to see how they develop.
The embryos will spend up to six days inside their own personal incubators, and you’ll be phoned each day with an update on both their progress and when the most suitable day for transfer might be (if you’re doing a fresh embryo transfer rather than a frozen one). Some embryos will be better quality than others, and it’ll be one of the good ‘uns that they transfer back into you.

Questions to ask your doctor at every stage of IVF treatment: free downloadable guide
IVF isn’t just overwhelming; it can also be a mind-boggling and sometimes terrifying experience because there’s so much to learn and so many rules to follow.
Problem is, doctors are busy – and they often don’t have the time to anticipate your concerns and provide all the information you might need.
This downloadable guide contains questions that will help you understand the process better, get the answers you deserve, and feel more in control of the situation (and your rights as a patient).
Enter your email address to receive it right away.
I won't send you spam. Unsubscribe at any time.
How does it feel in the hours and days after egg collection? Is it painful? What complications could arise?
According to most members of my helpful gang in the IVF forum, you’re likely to experience a certain level of discomfort afterwards – whether it be a small amount of bloating or fully fledged ovarian hyperstimulation syndrome (OHSS).
Here are their responses:
- “Moderate/severe OHSS! Ended up in hospital. There was always a big risk of me getting OHSS though (because my oestradiol level was high throughout IVF, and because I had so many follicles).”
- “I had bloating both times. After the first one I had very mild OHSS with extreme bloating, but luckily it went down so I could still have a fresh transfer.”
- “Bloating, cramping, tenderness, borderline OHSS.”
- “A little bleeding and soreness when going to the toilet. Became particularly uncomfortable to allow a full bladder to develop, but all resolved after a few days.”
- “There were no complications.”
- “Just a bit sore and bloated for a couple of days.”
- “The aftermath was tougher than I anticipated, due to mild/mod OHSS symptoms with a lot of bloating and constipation. Stomach swelled to about its largest five days later and I needed painkillers to get to sleep. Couldn’t crouch or bend over without pain/discomfort. Started to get self-conscious in the office.”
- “First time: no side effects. Second time: severe abdominal pain, ended up four days in hospital due to infection and mild OHSS.”
- “No complications, a little pain around my ovaries but nothing so bad I had to take pain relief for. This lasted about two days I guess. I was very bloaty but I think this was progesterone. I drank LOADS of water and no tea/coffee, and I think this helped a lot.”
- “I had some bloating and quite a bit of discomfort when moving around in the evening, but it began to ease the following day.”
- “I ended up getting an infection afterwards and was admitted to hospital for IV antibiotics. My main symptom was really bad stomach pain.”
- “Little spotting, pelvic ache. Nothing serious.”
- “I had constipation for a few days afterwards and I also got twinges and sharp stabbing pains for weeks afterwards – particularly when I sneezed, coughed or moved too quickly. I was lucky to get a BFP and at my seven-week scan. They said my ovaries were still the size of golf balls.”
- “Sore after and very bloated and constipated. No OHSS though. Had to resort to a load of prune juice to sort out the constipation. Had transfer on day 5. So glad as there was talk of day 3 transfer and I still felt awful that day.”
- “Just quite a bit of discomfort around my stomach.”
- “A few hours after the first egg collection, I became very sick, bloated and in pain, and was hospitalised for four days with mild OHSS. The second cycle I had no problems: felt back to normal straight away!”
- “Bloating and cramping.”
Can anything be done to reduce the risk of pain and complications after egg collection?
If you’re at risk of OHSS, read this article about how to avoid OHSS – or treat it if you do end up getting it.
Many of the treatments for OHSS can also be used for those who suffer from side effects but don’t have full-blown OHSS:
- Make sure you’re drinking enough water: your blood has lost a lot of fluid and is much more concentrated as a result, which makes your kidneys slow down (and can also cause dehydration). Water will help to rehydrate you and bring some fluid back into the blood. You ideally need to be drinking enough that you’re peeing out pale yellow urine every two hours.
If you read any American IVF forums, you’ll see that their health professionals recommend that you DON’T drink pure water – but have fluids containing electrolytes instead. (Gatorade gets mentioned a lot, and coconut water gets the nod from people who are freaked out by the sugar content and overall artificial-ingredientness of Gatorade.) That’s because they provide sodium and potassium – which are being lost in the fluid from your blood leaking out of your capillaries. British doctors tend to disagree with this advice.
- Take paracetamol or codeine to manage the pain (although if you think your constipation was bad before the codeine…).
- Buy some trapped wind tablets and laxatives in advance, in case you suffer from trapped wind and/or constipation after the egg collection.
- Avoid all strenuous activity to make sure you don’t accidentally get your now-MASSIVE ovaries in a twist (quite literally).
- Monitor how often you’re urinating, and what colour your urine is: dehydration is a sign of OHSS.
- Get yourself to a doctor (or hospital) if your weight is increasing significantly and you’re not urinating anywhere near as often as normal.
In summary… IVF egg collection: not the most amazing experience of your life, but unlikely to be the worst, either
As you can see, most people experience some level of discomfort at some point during the egg collection process – but for most, it’s only a small amount of pain and/or bloating, which can be managed with the help of painkillers and/or prune juice/laxatives.
If you feel significantly bloated or in pain, you could have OHSS; call your hospital or clinic to find out what to do.


