IT DOESN'T MATTER WHETHER YOU'RE TRYING TO CONCEIVE NATURALLY OR VIA FERTILITY TREATMENT: if you have low-quality eggs, or a low egg count, or a combination of the two, things become jolly difficult.
The term “ovarian reserve” relates to both the quality and the quantity of your ovarian eggs – and both are important when it comes to getting pregnant. Age is the biggest determinant of ovarian reserve: the older you are, the lower it’ll be. If you’ve just started secondary school and you’re reading this article for some reason, now might be the time to start scouring the playground for potential sperm donors/fathers. Just kidding. I was totally kidding. I really need to stop making jokes like this.
Anyway! Here are some questions you might have about eggs – and my attempts to answer them in a way that’s easy to understand without resorting to horrendous jokes.
How many eggs do I start with? And how quickly do I lose them?
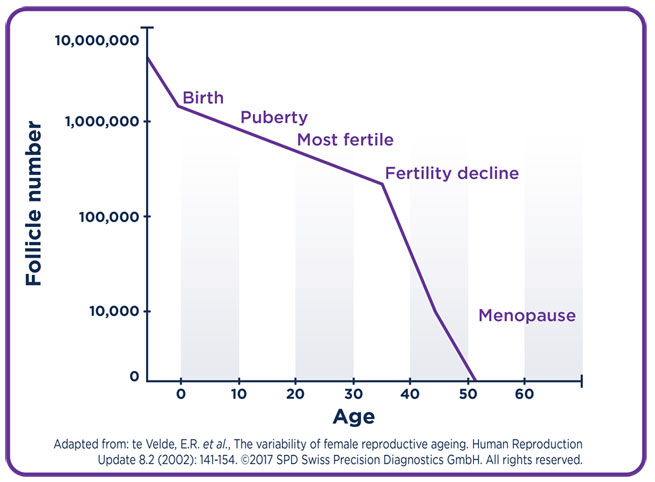
You’re born with all the eggs you’ll ever have, and there are an awful lot of them: approximately two million. But it’s not the case that you’ll lose one egg a month from puberty onwards and still have a repository of just under two million left over when you’re 84.
In fact, you’re pretty much constantly losing eggs – even when you’re still a child. By the time you hit puberty, you’re already down to your final 350,000 or so eggs – and then every month after puberty you’ll continue to lose about 1,000 eggs.
What happens to all the eggs? Well… during the average cycle, FSH is released to stimulate the growth of a small number of egg-containing follicles in the ovaries. Only one of the egg-containing follicles will grow to be big and strong enough for fertilisation – and therefore only one egg will be released into the fallopian tube. All the others will die off.
So how do we get to the “1,000” number? Well, in addition to those few “stimulated” follicles that die each month, you also lose almost 1,000 other eggs. Every single cycle.

If I’m consistently losing 1,000 eggs a month, what changes at the age of 35 to cause all the “ooh you’re too old now” scare-mongering?
At the age of 35, surely you’re just 12,000ish eggs down from where you were at the age of 34, right? Wrong: the rate of egg depletion increases as you age. By the time you’re 30, you’ll have about 12% of your eggs left. When you get to 40, you’ll be down to your final 3%. A few years later and they’ll mostly all be gone. (Menopause is typically between the ages of 48 and 55.)
You won’t suddenly start dropping a load more eggs as soon as you’ve made a wish over the 35 candles squished onto your birthday cake, but doctors tend to use that age as a shortcut to determining your likelihood of conceiving both naturally and with fertility treatment. Some clinics and hospitals will use the age of 37 or 40 instead.
(Of course, women don’t all begin life with the exact same number of eggs. And the rate at which they lose them differs slightly too: it’s all down to the natural inclinations of the body, and it’s why women go through menopause at slightly different ages.)
I started my periods really young; will that affect the age at which I lose all my eggs?
No. As we’ve seen, women lose THOUSANDS of eggs all the time – even before they hit puberty. An extra few eggs that die as a result of two extra years of menstruation means nothing in the grand scheme of things.
The same explanation goes for women who’ve spent many years on the pill: they’ll have lost thousands of eggs a month anyway, so a few hundred “saved” eggs (through not ovulating) means nothing really.
Is there anything I can do to slow down egg loss?
The number of eggs you’re born with and the rate at which you lose them is pretty much set in stone: lifestyle factors don’t really get a look-in.
Except for just ONE lifestyle factor, that is: smoking. Practically all scientific studies show that smoking accelerates the loss and quality of eggs – and as a result, it may also bring forward your menopause by several years too.
Two other factors to be aware of are radiation therapy and chemotherapy: both have been shown to reduce the quantity of eggs.

Can I find out how many eggs I have remaining?
Not directly. But a few different tests will give a good indication of whether you have “a lot” or “not a lot” of eggs left.
Find out more about them here:
Where/how do I get these tests for egg quantity?
If you're having IVF treatment, you'll be given these tests right at the start – whether you're on the NHS or paying privately. (Find out more about “day 3″/baseline scans here.)
But what if you've been trying for a baby for a while but think it's too soon to start considering IVF? Or you have a history of early menopause in your family and want to see if it's likely to affect you too? Or you don't want to have a baby yet, but would like to know if time is on your side?
If you want to check your egg quantity/count in those scenarios, you'll have to go private.
Most private fertility clinics offer “ovarian reserve” testing for about £450/£500. It usually involves blood tests for oestradiol, FSH and AMH levels, plus an antral follicle count scan (which is exactly the same batch of tests you'd get at the start of IVF treatment).
Alternatively, it's possible to buy at-home AMH tests – which are much cheaper (they cost about £100). AMH levels are considered the most “useful” of the hormones to test, and at-home AMH tests are believed to be as accurate as the clinic versions. AMH tests won't give you the whole picture because they can't tell you about egg quality (read below for more on this), but then the ovarian reserve tests offered by clinics can't tell you about that either.
One important thing to mention: when fertility clinics provide ovarian reserve tests, they'll do an “antral follicle count” scan too. The antral follicle count is one of the best ways to measure egg quantity, but you definitely can't do that one at home.
As long as you're aware of the drawback(s) of at-home AMH tests, I don't see any harm in using them – especially if you're older than 35 and have been trying for a few months without success. An at-home test could give you the information you need to approach your GP and ask for further investigations.
There are a few companies out there providing at-home AMH tests, but the one I recommend is called LetsGetChecked. They have a team of doctors who'll review your results before sending them out, and nurses are available 24/7 in case you want to discuss your results after receiving them. The tests are super easy to use, and thoroughly non-fiddly!
If you enter the code “theduff” at checkout, you'll get 15% off your AMH test (and any other test you order).
What’s the deal for younger people who have a low supply of eggs?
Some younger people also – for various reasons – have a supply problem when it comes to their eggs. But they’re likely to have good-quality eggs, which means that (as we’ll see) they have a far better chance of conceiving.
Fertility doctors will help you figure out the cause if you don’t know what it is already.

Questions to ask your doctor at every stage of IVF treatment: free downloadable guide
IVF isn’t just overwhelming; it can also be a mind-boggling and sometimes terrifying experience because there’s so much to learn and so many rules to follow.
Problem is, doctors are busy – and they often don’t have the time to anticipate your concerns and provide all the information you might need.
This downloadable guide contains questions that will help you understand the process better, get the answers you deserve, and feel more in control of the situation (and your rights as a patient).
Enter your email address to receive it right away.
I won't send you spam. Unsubscribe at any time.
Even if I’m over the age of 35, I’ll still have a few thousand eggs in there – so what’s the big deal? I only want one or two kids, after all…
If you’re over the age of 35, you don’t just have a smaller collection of eggs to work with. Successful fertilisation and implantation requires high-quality eggs, but the majority of your eggs will be of the “low quality” variety. (Think of them as hanging around in a humid environment, slowly stagnating. Or maybe don’t.) So you have a double whammy of a problem: there are fewer eggs to be fertilised, and many of those eggs are more likely to be a bit rubbish.
If you’re trying to get pregnant naturally (and you know you don't have any other fertility issues), you’ll struggle. If you’re trying to get pregnant via IVF treatment, it’ll be a harder task than it is for younger people. Why? Two reasons:
- With a “normal” menstrual cycle, one “mature” egg gets released into the fallopian tube each month, ready for fertilisation. With IVF, the aim is for you to grow as many mature eggs as possible so that those eggs can be collected by doctors and fertilised in a lab. (More eggs = more opportunities for at least one to fertilise.) If you don’t have many eggs in the first place, your body will find it tougher to get a large number of them to reach maturity in one go – even with the help of fertility meds.
- The eggs you do manage to produce are less likely to be good quality.
That’s why fertility clinics often won’t treat older women who are trying to get pregnant using their own eggs. This chart (from advancedfertility.com) helps to explain things:
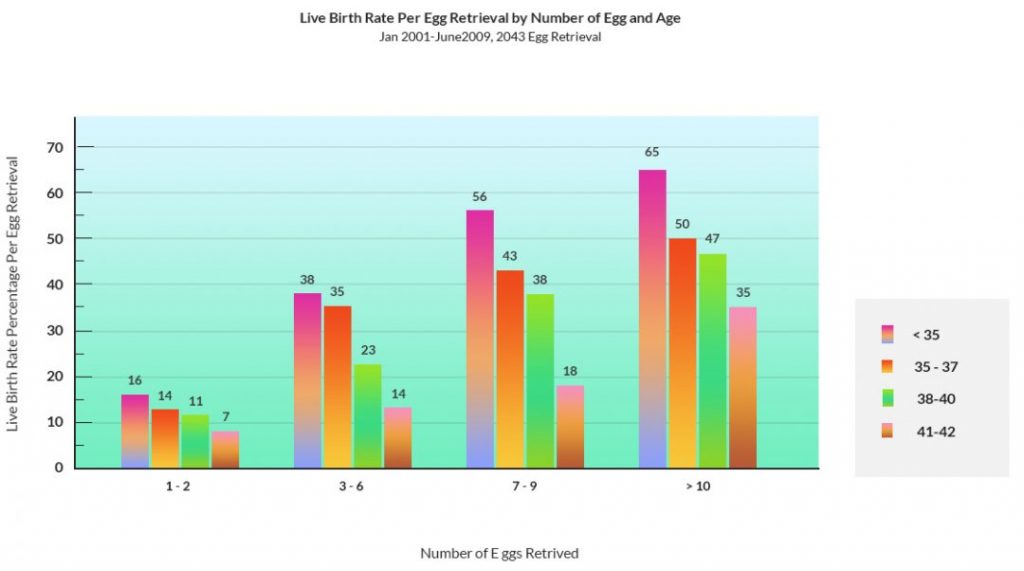
Basically: older women tend to have fewer eggs retrieved, and even when eggs are retrieved, the live birth rate is much lower than for younger women (a result of poorer egg quality).
Tell me more about “egg quality”. What exactly does it mean?
An egg is either “good quality” or “bad quality” – there’s no “so-so quality” or “I-guess-it’ll-do quality”.
A bad-quality egg:
- Won’t fertilise, OR
- Won’t implant if it does fertilise, OR
- Has a higher likelihood of being miscarried if it does implant, OR
- Has a higher likelihood of having a genetic disorder such as Down Syndrome if it does survive to term
If you’ve ever wondered why we see more cases of infertility, miscarriage and genetic disorders in older women, that’s your reason: bad-quality eggs leads to those particular outcomes.
If you want to know the science behind it, there are two main causes of a bad-quality egg:
- Lack of energy (seriously!). Each of your eggs contains mitochondria, which can be thought of as teeny tiny batteries. When an egg is fertilised, it’s the mitochondria that give it the energy it needs to constantly divide and eventually become a foetus. As you age, these mitochondria produce less and less energy. The result? Even if you have a successfully fertilised egg on your hands, it may simply run out of steam before it’s able to divide.
- The “wrong” number of chromosomes. An egg needs to have the correct number of chromosomes in order to develop into a healthy, genetic disorder-free baby. As you age, more and more of your eggs will contain the “wrong” number of chromosomes. If you want all the details about why and how this happens, here you go! (It took me forever to write up the information, so pretty please do pretend to read it and be fascinated by it.)
A good-quality egg doesn’t come with these problems – and about 80–90% of a 20-year-old woman’s eggs are good quality. As we age, our eggs also age – and by the time a woman is 44 years old, only about 20% are good quality. (And remember: that’s 20% of a much smaller number of eggs.)
Is it possible to determine the quality of my eggs?
It’s kind of possible to guesstimate the quality of your eggs by looking at a few factors:
- Your age. Nearly all women under 35 will have good-quality eggs.
- The number of eggs you have left – as indirectly determined by blood tests for FSH, AMH and oestradiol levels, as well as an antral follicle count. This usually comes down to age again: if you don’t have many eggs left, it’s probably due to how old you are – and that affects the quality of your eggs too. If you’re young and a smoker, you’ll also have a reduced egg count compared to the norm, and the quality of those eggs will be worse.
- The outcome of any recent pregnancies. If it takes you a long time to conceive or you’ve suffered early miscarriages, it could mean decreasing egg quality.
- The outcome of any recent IVF attempts. If none/very few of your eggs were successfully fertilised – or if you constantly had problems getting fertilised eggs to implant – it might indicate a problem with egg quality.
- The results from pre-implantation genetic screening (PGS). The screening identifies chromosomal abnormalities in embryos, so you’ll need to already be having fertility treatment like IVF to participate. A high number of abnormalities in your embryos is an accurate predictor of the quality of your eggs in general. (Over 90% of chromosomal abnormalities are thought to come from the egg rather than the sperm.)
(Note that the HFEA currently doesn't recommend PGS. I've written a detailed post about the pros and cons of PGS testing here.)
Does anything other than age affect egg quality?
Yup. In fact, younger people can have poor-quality eggs too – and it’ll also affect their success rates with getting pregnant naturally or via fertility treatment. (Having said that, it won’t affect their success rates to the same extent as older people, because they’re more likely to have more good eggs somewhere among their abundant collection).
In addition to age, egg quality is affected by the following:
- Smoking
- Drug use
- Endometriosis
- Ovarian cysts
- Obesity
- Some immunological disorders
- Radiation therapy and chemotherapy
Age is the most important determinant – so you’re unlikely to improve the quality of your eggs through lifestyle changes if you’re totally over the hill (which in this context is your mid-40s onwards).
But if you’re in your 20s to early 40s, you can improve the quality of your eggs by losing weight if your BMI is over 30, and by quitting smoking and drug use.
Remember: if you’ve been struggling to conceive and you make these lifestyle changes, you might not actually need fertility treatment at all. And if you do need fertility treatment, it’s more likely to be successful.
Is there anything else I can do to improve egg quality? Incense? Crystals? Chanting? Anything?
If you google the question, there’s PLENTY you can do – but most are pure hogwash. (Seriously: going gluten-free won’t do anything other than diminish your mermaid-themed-nursery fund and make you crave real bread.)
But there are a few suggestions that fertility specialists either support or believe won’t have any adverse effects – so there’s no harm in trying them. They are:
- Get your hormones more balanced by de-stressing, sleeping well, and regulating your blood sugar.
- Give your mitochondria more energy by taking CoQ10 as well as vitamins A and E.
- Neutralise free radicals in your body (which speed up the ageing process of your eggs) with a diet rich in antioxidants, e.g. brightly coloured fruit and veg, green tea and – in moderation – red wine.
- Start taking a B vitamin called Inositol, which is thought to improve egg quality by increasing insulin sensitivity of the ovaries.
- Talk to your doctor about a hormone called DHEA (dehydroepiandrosterone): recent studies indicate that it may improve egg quality, but it’s a pretty potent hormone and needs to be taken under supervision.
If I have (or probably have) poor-quality eggs, will IVF help?
That depends. If the poor quality is down to advanced age, there’s a chance you’ll be refused fertility treatment because you also have very few eggs to work with.
The chart below from the Human Fertilisation & Embryology Authority (HFEA) shows just how much age affects your chances of successful IVF. (I'm hoping that a more up-to-date chart will be published soon.)
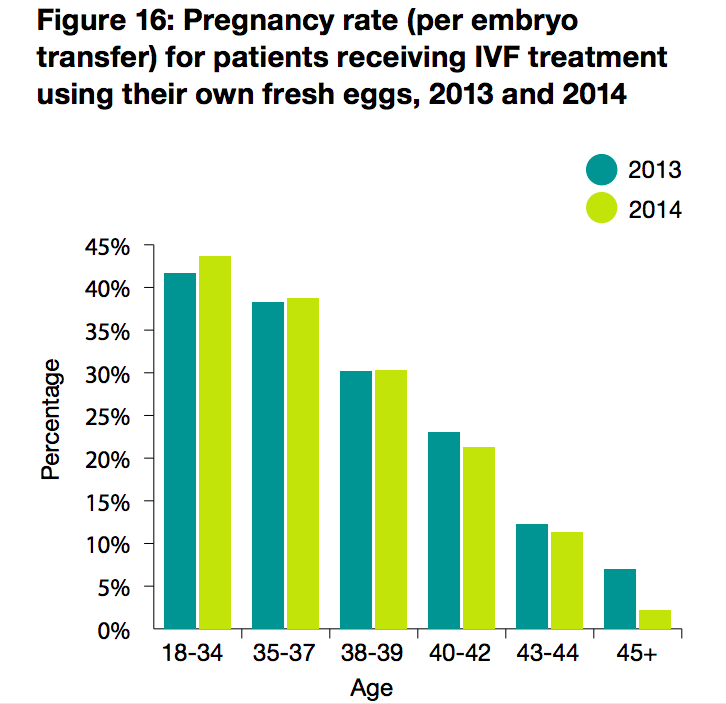
<slight diversion> Are you wondering why pregnancy rates seem to be decreasing year-on-year in older age groups? I had the same question. The answer may lie in a separate HFEA report I found online (unlike the chart above, this explanation is about births rather than pregnancies, but the gist is the same): “If there is only a small number of women in an age group it can make results appear to be very changeable, when expressed as a percentage. For instance, one year we may see that from 1,000 cycles performed in the youngest age group, there were 300 live births. This would give a live birth rate of 30%. We may see in the same time period that only 10 cycles were performed in the oldest age group, three of which resulted in live births. This also results in a live birth rate of 30%. If the number of cycles stayed the same in the subsequent year, but one less woman in each age group had a live birth, the percentages would change to 29.9% for the younger women (barely changing), and to 20% for the older age group (it appears the rate has dropped dramatically). As larger groups are less affected by small changes (possibly caused by chance occurrences), they tend to remain steadier.” </slight diversion>
If you’re still young and struggling to get pregnant as a result of poor-quality eggs, there’s a good chance IVF will help. There are a couple of reasons why:
- With IVF, the aim is for you to grow as many mature eggs as possible, so that those eggs can be collected by doctors and fertilised in a lab. More eggs = a higher chance that at least one of them will be of the high-quality variety.
- Your embryos can undergo preimplantation genetic screening (PGS) to check for abnormalities – which increases your likelihood of a successful pregnancy because only a healthy embryo will be put back in. As I noted above, PGS is still very much a controversial practice – and not everyone agrees that it improves your likelihood of pregnancy. Read all about PGS here.
There’s a lot of information here. If you could summarise everything for me, that’d be great…
- Egg quantity AND egg quality are important when it comes to fertility. Collectively, they're known as “ovarian reserve”.
- You can’t do anything about the number of eggs you have left (other than to give up smoking).
- But you can take steps to improve your egg quality – and doing so will actually make it easier to conceive naturally, meaning you may no longer need fertility treatment.
- But age trumps everything: if you’re over the age of 35 (and particularly if you’re over the age of 40), you’ll struggle to improve your egg quality in a way that overrides the loss in quality caused by age.
- If you’re relatively young and you have either poor-quality eggs or not many of them, you have a better chance of conceiving (either naturally or through fertility treatment) compared to older women.
Questions to ask your doctor at every stage of IVF treatment: free downloadable guide
IVF isn’t just overwhelming; it can also be a mind-boggling and sometimes terrifying experience because there’s so much to learn and so many rules to follow.
Problem is, doctors are busy – and they often don’t have the time to anticipate your concerns and provide all the information you might need.
This downloadable guide contains questions that will help you understand the process better, get the answers you deserve, and feel more in control of the situation (and your rights as a patient).
Enter your email address to receive it right away.
I won't send you spam. Unsubscribe at any time.


